As Dr. Jay Fisher drives to work on the evening of Jan. 10, he fully recognizes the fact that he may have to act quickly to save a child’s life during the next 10 hours. Conveying a strong sense of responsibility, Fisher begins to draw upon more than two decades of experience as a pediatric emergency medicine physician, visualizing a variety of life-threatening scenarios and the steps he will take to preserve the lives of his young, often-fragile patients.
As the medical director of the Pediatric Emergency Department for Children’s Hospital of Nevada at UMC, the 54-year-old physician understands the importance of mental preparation, and his unique approach to visualization went on to play a crucial role in treating a severely ill 1-month-old patient during his overnight shift.
“When you go into this field, you recognize that there are going to be instances in which a child’s life hangs in the balance,” Fisher says prior to beginning his work for the day.
“I always test my mind and think things through before each shift.”
“He really embodies heartfelt compassion,” says Irma Albarran, a registered nurse who has worked alongside Fisher for more than eight years. “You can see it in his eyes. He makes us remember why we do this.”
Throughout the night, Fisher puts his patients and their parents at ease as he tends to injured and ill children within the emergency department.
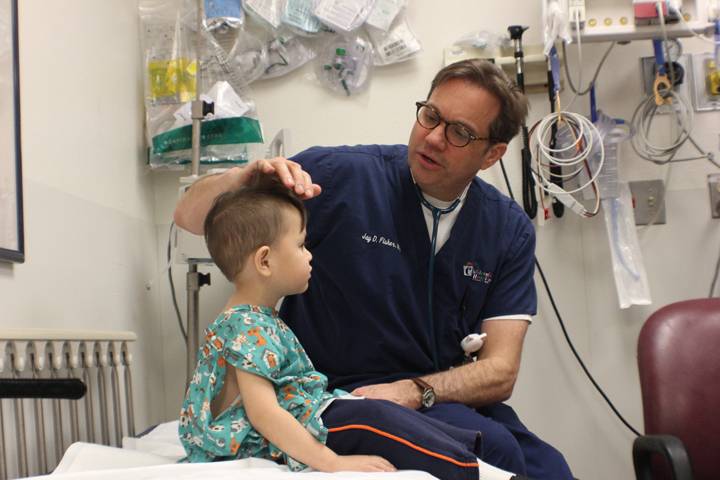
While examining 3-year-old Bruce toward the beginning of his shift, Fisher shows his dedication to comforting children and their families. Bruce giggles throughout the examination as Fisher makes funny faces and asks questions to forge a strong connection with the young patient. Bruce’s eyes light up when Fisher begins using a reflex hammer during the exam.
“Do you want to try it?” Fisher says as he hands the small, rubber instrument to the child.
Prior to the examination, Fisher has an in-depth conversation with Bruce’s mother, Amber, who explains that her son hit his head on a tile floor and was unresponsive for less than one minute. In an effort to check for a potentially dangerous brain injury, Fisher plays a number of games with Bruce that help identify the integration between the child’s cerebral cortex and cerebellum. After asking the child to kick the doctor’s hands while lying down, Fisher instructs Bruce to hop down from the bed. “Can you stand on one foot like Bruce Lee?” Fisher asks the talkative child, who is named after the well-known martial artist. “I appreciate that he talked to Bruce on his level,” Amber says. “So many times, doctors only talk to the parent and don’t pay attention to small children.”
Following a reassuring examination, Fisher sits down with Amber and discusses the risks and benefits associated with performing a CAT scan. Both Fisher and Amber express concerns about exposing the child to a high amount of radiation at such a young age, and they come to a shared decision. Rather than performing a CAT scan, the family will wait in the emergency room a bit longer to ensure Bruce does not exhibit any symptoms of a serious injury. “I appreciate that he is not rushing to do potentially dangerous tests,” Amber says.
Even after more than two decades of working as an emergency medicine physician, Fisher strives to connect with his patients and serves as an example for his fellow physicians, says UMC Director of Emergency Services Katie Ryan. “He can still truly be touched by a patient,” she says. “He is one of the most compassionate physicians I have ever worked with. No matter how busy he is or how tired he is, the individual patients will never notice because he is very attentive.”
While the night begins with a steady flow of patients, the volume increases significantly approximately six hours into Fisher’s shift. The emergency room experiences an influx of patients, including Faith-hope, a 1-month-old girl experiencing unexplained episodes of apnea. Faith-hope’s mother, Theresa, explains that the baby stopped breathing several times, turning blue in some instances. After speaking with Theresa and thoroughly examining the child, Fisher orders tests for influenza and respiratory syncytial virus (RSV), in addition to a chest x-ray, hoping to determine the cause of her condition.
Less than one hour later, Faith-hope stops breathing again. With his patient experiencing episodes of apnea, Fisher’s bright smile quickly fades away, revealing the stoic face of a man with a singular focus. He acts quickly, using one of the key scenarios he visualized prior to the beginning of his shift. He lifts the infant’s jaw to keep her tongue off of the back of her throat and utilizes a bag valve mask to provide her with oxygen. After Faith-hope resumes normal breathing, Fisher turns to Theresa, who is visibly shaken by the frightening situation, tears running down the sides of her face. “We’ll get to the bottom of this,” Fisher says, comforting the mother by expressing his confidence in the team at Children’s Hospital of Nevada at UMC.
Fisher’s words are proven true approximately five minutes later, when registered nurse Brittany Perez informs the team that Faith-hope tested positive for RSV, a common respiratory virus. Fisher describes the situation to Faith-hope’s family in great detail, explaining that the child will be transferred to the hospital’s Pediatric Intensive Care Unit, where she will receive a high flow of oxygen to prevent additional episodes of apnea during the treatment process.
While Theresa remains concerned about the condition of her young daughter, she is comforted by the fact that Fisher and his team were able to quickly identify the source of Faith-hope’s apnea. Theresa has visited the Children’s Hospital of Nevada at UMC Pediatric Emergency Department several times, and she describes Fisher as a compassionate and extremely informative physician. “He makes sure that you get the answers you need,” she says shortly after arriving in the emergency department with her daughter. “He is just an all-around good doctor. Because of the way he is, I feel comfortable coming here. I drove across town to come here.”
As the emergency department continues to experience a surge in patient volume, Fisher expresses his concerns for the future well-being of a 15-year-old patient who arrived at the emergency room earlier in the evening after being found intoxicated and transported by EMS workers. A test revealed that the teenager’s blood alcohol content was approximately 3.5 times the legal limit. “I hope this is a teachable moment. He came dangerously close to a situation that could have been lethal,” Fisher says. “We have seen many kids die of blood alcohol poisoning.” In an effort to prevent similar experiences in the future, Fisher speaks to the teenager’s parents in Spanish and provides them with a referral to an adolescent medicine specialist for follow-up care.
Throughout the evening, Fisher works alongside Dr. Kevin Mailland, a third-year family medicine resident at the University of Nevada School of Medicine, providing the younger doctor with key insights on a variety of cases. “I really appreciate the time he takes to teach you,” Mailland says.
Fisher’s wealth of experience serves as a valuable asset to team members and patients alike. “It’s OK sweetie pie. You’re a good girl.” Fisher says with a warm smile as he gently examines the ears of 3-month-old Jasmine, who came to the emergency room with her young parents after crying frequently and experiencing difficulty sleeping. Offering the family his undivided attention, Fisher sits on the small bed of the exam room, explaining the many potential causes of Jasmine’s discomfort and providing a sense of relief to the parents. “I have examined 100,000 children in my career, and this is a healthy baby,” he says, exuding the confidence that comes with decades of experience treating children.
“Her examination is very reassuring.”
Following a long and busy night shift, Fisher prepares to go home. He reviews the current cases and takes a moment to thank all of his team members for their hard work. Before traveling home to have breakfast with his wife, Fisher expresses pride in the team at Children’s Hospital of Nevada at UMC and the important role they play in keeping children healthy. “I have the best team in the city,” he says.
While Fisher has reached the end of his shift, he never truly separates from his work. Much like a concerned father, Fisher frequently thinks about his patients and wishes the very best for the children as he sends them back into the world.